Over the last few weeks, nine CMF members have been working in Haiti, as part of a Samaritan’s Purse team helping with the fight against cholera.
We’ve been hearing from Abi Boys (whose posts are below), but just before the end of the trip we had another update from Alex Bunn, who has a portfolio career which includes being the CMF student Southern Team Leader. Alex writes:
 Treating cholera – the Nokia sign
Treating cholera – the Nokia sign
“So what is it like to treat cholera? I had only read about it before in textbooks, out of historical interest. We do have the infamous cholera beds here, with a hole in the middle to allow discreet ablutions without the patient having to rise, which would be risky with such fluid depletion. One patient yesterday received his 90th bag of Ringers Lactate in just 3 days. But thankfully, a good proportion of patients manage on Oral Rehydration Therapy alone. In fact, they reckon only 7% cholera patients need admission. Which means most patients simply have a self-limiting ‘touch of cholera’, a phrase which seemed absurd before we saw the range of severity in practice. One sign of dehydration I had never seen before in adults is sunken eyes, which can be quite dramatic. I also had never seen jaw dislocation secondary to vomiting. Pulse on the other hand is virtually never useful as a gauge of severity, unless it is absent! Is relative bradycardia a result of the very common hypokalaemia? We have no blood tests in the treatment camps, but early surveys suggested potassium levels are commonly in the low 2s. We avoid replenishing too rapidly as renal impairment is a likey snare early on, and with inexperienced nursing staff it seems safer to restore it orally where possible. Another sign that seems quite useful is the Nokia sign: even the poorest seem to carry phones, and once they are on their mobiles, they are home and not-so-life-threateningly dry.
Mortality down – cholera songs
We think that the mortality rate has dropped off partly as patients are brought in earlier. Initially, 30 patients per hour were being brought in on wheelbarrows and slumped on motorbikes. But public broadcasts have encouraged safer water treatment and early ORS to reduce the incidence. The Bercy camp even employs an educator to sing his cholera prevention song through a megaphone at regular intervals through the day! Sadly, one local staff member did not heed the advice, and perhaps out of shame did not seek medical attention and died.

Fear and stigm
a were rampant. A cholera centre run by another NGO was burned down by locals fearing it would attract cholera into their neighbourhood. Samaritan’s Purse has worked hard in local partnerships. One example is that the security teams are recruited from all the local rival gangs, to avoid territorial disputes. And training Haitian medical staff for the future is a key priority at all the centres.
Unexpected extras – meths poisoning
But it’s not all cholera here. Two days ago I was asked to help investigate rumours of a new outbreak of an unknown illness with headache and vomiting that had rapidly killed twenty people in two villages. Was it meningitis, dengue, or perhaps typhus? That’s all they need, we thought. But it was good to see the array of NGOs collaborate here, and share intelligence by text and email. We visited one village to interview the relatives. As we talked to the family on their porch, a crowd of 30 quickly gathered, including the police chief and multiple interpreters. Not an easy environment to take a sensitive history.Thankfully, it did not seem to be a febrile illness as expected, and the common factor was blindness and death within hours. Sadly, the most likely cause was methanol poisoning from a batch of home-made hooch. An epidemiologist from CDC established the same cause in the other village later that day. Its easy to blame the amateur brewer, but in a country with such basic education, perhaps its no surprise.
Tragedy and hope – ‘Love in the time of cholera’
There is a strange blend of tragedy and hope here. Today we met a 5 year old boy who presented with yaws, but was markedly withdrawn. It transpired that most of his family were killed in the earthquake one year ago, and he had been wandering the streets, fending for himself until just last week, when an aunt recognised him and took him in. You can imagine how traumatised he must be. Yet many Haitians have remarkable resilience and faith. The lu
nchtime worship in the cholera tents puts our Sunday services at home to shame. If they can lose half their family, live in abject poverty (in part due to reparations forced on them by a colonial power for loss of slave earnings), contract cholera, but still sing over the vomit bucket with more vigour and thankfulness than a prosperous Westerner, what does that say about my faith in comparison?”
Alex Bunn, Saturday 29 January 2011, Haiti
For more details on Samaritan’s Purse go to www.samaritans-purse.org.uk
___
Here is Alex’s earlier post.
Alex writes: ‘I’m taking a day off today, so finally have a moment to reflect. It’s quite a tight schedule, up at 5am to arrive before sunrise at the cholera camp, back at 7:30pm. We avoid the roads in daylight hours partly for security. It was quite unnerving on the first day to see a couple of guys on motorbikes speed past our Landcruiser brandishing guns, until we realised they were our armed escort! With any news about the elections there are rumours of unrest that may boil over into riots or ‘manifestations’ on the streets.
That would mean a lockdown at the clinic too, but so far we have been spared.
One abiding memory of the camp will be the ubiquitous bleach. Every time we leave a ward we have to splash through trays of it. My trainers have never shone so white! And there’s a tank of 0.2% stationed at every gateway, where an attendant barks “WASH! WASH!” at all who pass. They should try that strategy in the NHS! Quite a sweet gesture from the chaplains: every night they are waiting to greet us with bleach brushes to decontaminate our shoes one more time. It seems a fittingly Levitical role for a pastor!
It is quite a luxury to be so selective in our admissions: no enteropathy, no entry! Although we get an occasional hint about the struggling state sector when we receive the overflow from their overwhelmed clinics. And there is a hint of sadness in the eyes as the numbers wane: many staff here don’t have regular work, so the end of an epidemic might spell unemployment for many of them. Long term, economic restructuring is going to be the greatest need, one that won’t respond so easily to the good
will of a few volunteers. Lets keep praying!’
Alex Bunn, Friday 21 January 2011, Haiti.
___

Abi Boys is another of the nine CMF members helping with the fight against cholera in Haiti.
She’s been telling us about the political and clinical challenges facing their team.
Abi writes: ‘As we pass the 200,000 mass grave for earthquake victims, our Haitian driver and security guard sing along in French to an anthemic Celine Dion tune. But the back of the minibus is silent. Dusk is
falling, and we’re on our way from our compound to the cholera treatment centre, right in the midst of the Cité Soleil slum. Each of us is reflecting on the gravity of what we’ve just passed and the anticipation of the dehydrated patients the night promises to bring. It often feels like work in Haiti is damage limitation; it’s hard to know where their hope will come from.
Speaking with the locals, there’s a feeling the forthcoming election won’t provide them with hope for the future. There’s anger at the KEP (the election company) and wanting to do away with President Préval – reflected in the graffiti you can see at the police check point ‘ABA KEP, arrete Préval’ which I’m told means ‘go away K.E.P and stop Préval – put him in jail’. And yet they don’t seem happy with any candidates – the two remaining candidates are a university teacher (Mirlande Manigat) and a singer (Michel Martelly). The word on the street is that the singer will win because people feel uplifted by him, but they don’t expect he can run the country!
We arrive at the heavily secured treatment centre, one of the poorestand gang heavy regions of Haiti. Immediately we bleach our hands and go to our container where we can leave our things (and the only place we are allowed to eat or drink). The layout of the centre is separated into a triage area, resuscitation area and wards divided into male, female and children. Between each zone are bleaching handwash and foot trough stations, manned by staff who yell ‘wash’ in case you try to pass without decontaminating. Thankfully the cholera numbers are diminishing, but we are still getting patients brought in at the brink of death.
Halfway through the night we’re informed by security that there’s some gang activity outside (retribution for an attack the previous night), and it’s likely there’ll be gunshots. We’re condensed into a retreated position inside our compound to avoid stray bullets. 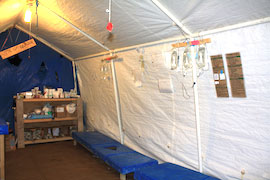 As the cholera ‘epidemic’ is being downscaled to just ‘endemic’, it’s clear this is just one of many challenges the Haitians are having, and have had, to deal with. Local staff are afraid; some of our patients do not want to leave because they feel safer in our compound. I wonder how many insults the Haitian people can withstand, resilient as they seem? They say the change must come from the people themselves. Certainly it would be helped by a stable government and responsible President.
As the cholera ‘epidemic’ is being downscaled to just ‘endemic’, it’s clear this is just one of many challenges the Haitians are having, and have had, to deal with. Local staff are afraid; some of our patients do not want to leave because they feel safer in our compound. I wonder how many insults the Haitian people can withstand, resilient as they seem? They say the change must come from the people themselves. Certainly it would be helped by a stable government and responsible President.
The chaos and corruption in the first election, the surprise arrival of ‘Baby Doc’ [former president Jean-Claude Duvalier], and the piles of rubble across the country, make you think progress is still decades aw
ay. But when I see aid organisations empowering a community; when I look at an individual or a family – collecting water, eating well, finding shelter, kids going to school – there’s a feeling that the grassroots people may just be the ones to turn things around.’
Abi Boys, Wednesday 19 January 2011, Haiti.
___
Here is Abi’s first blog post from Haiti, received on 17 January:
Abi writes:
‘I was impressed
as we arrived at the massive, floodlit 240 bed purpose built cholera centre (run by Samaritan’s Purse) that the banner outside declared “Cholera Treatment and Prevention Centre”. And it is largely due to the simultaneous prevention and treatment approach that the epidemic numbers have dropped over the past few weeks. Basic disease and hygiene education have led to restricted spread, families recognising the symptoms and bringing patients in earlier – so intervention (getting IVs in) is easier, and improved response rates. I understand the mortality rates have been kept below average (normally 2%, in our clinic around 0.5%)
 During the night shift in the admissions area we saw some people presenting with early or mild to moderate cholera who could be trialled to see if they responded to Oral Rehydration Solution alone. Those who present with severe, frequent vomiting and diarrhoea (watery and white – to distinguish it from typhoid or other infection) go straight to the IV tent, where immediate fluid resuscitation is started. Vast, vast quantities are essential to retrieve these patients and secure survival. Once a few litres are in, within the first hour, there is often very quick transformation. A great relief to see a patient who was lethargic, sunken eyes, unaware and unbothered by our attempts to put a cannula in, and become awake and thankful to be alive!
During the night shift in the admissions area we saw some people presenting with early or mild to moderate cholera who could be trialled to see if they responded to Oral Rehydration Solution alone. Those who present with severe, frequent vomiting and diarrhoea (watery and white – to distinguish it from typhoid or other infection) go straight to the IV tent, where immediate fluid resuscitation is started. Vast, vast quantities are essential to retrieve these patients and secure survival. Once a few litres are in, within the first hour, there is often very quick transformation. A great relief to see a patient who was lethargic, sunken eyes, unaware and unbothered by our attempts to put a cannula in, and become awake and thankful to be alive!
Once stabilised, the patient is transferred to the men’s, women’s or children’s wards. The set-up has to be basic and systematic. Beds lined up with crude holes in the centre for the frequent passing of waterfall stools, three buckets; one beneath the hole, one to change over when it’s full, and one by the head for vomiting. Fluid management is monitored on at least an hourly basis. Most are in hospital for 2 to 3 days. Lives are being saved!’
Abi Boys, Monday 17 January 2011, Haiti.



